Diabetes is one of the defining health challenges of our time. It affects people of all ages and backgrounds, in every region of the world, and its prevalence is rising at a pace that healthcare systems are struggling to keep up with. For the hundreds of millions of people living with the condition, and many more at risk, the need for better treatments and continued research has never been more urgent.
Key Takeaways
- According to the International Diabetes Federation, nearly one in nine adults worldwide is currently living with diabetes, and this number is projected to rise significantly by 2050.
- Diabetes places an enormous human cost on individuals and families, with serious complications affecting the heart, kidneys, eyes, and nervous system.
- Current treatments manage diabetes effectively but fall short of a cure, leaving patients dependent on lifelong therapy.
- Both type 1 and type 2 diabetes research are advancing rapidly, with stem cell-based approaches emerging as the most promising new diabetes treatment avenue toward a functional cure.
- Companies like RMS are working to develop scalable, accessible therapies that could transform the lives of people with diabetes worldwide.
The Rising Global Prevalence of Diabetes
The scale of diabetes as a global health issue is difficult to overstate. According to the International Diabetes Federation’s 2025 Diabetes Atlas, approximately 589 million adults between the ages of 20 and 79 are currently living with diabetes worldwide; that’s roughly one in nine of all adults in that age group. Projections suggest that figure could climb to around 853 million by 2050, an increase of nearly 50% in just 25 years.
What makes these numbers particularly alarming is how much of this prevalence goes undetected. The IDF estimates that more than four in ten people with diabetes are currently unaware they have the condition, meaning they are not receiving treatment and are at heightened risk of serious complications. Many will only receive a diagnosis once those complications have already begun to develop.
The global diabetes prevalence spans every region and income level. Estimates of its scale vary depending on methodology and the population measured; a 2024 Lancet study found that more than 800 million adults aged 18 and over were living with diabetes in 2022, while the IDF’s 2025 Diabetes Atlas, which measures adults aged 20–79, puts the figure at approximately 589 million. The difference reflects distinct methodological approaches rather than contradictory findings, and both point to the same conclusion: diabetes affects an enormous and growing share of the world’s adult population. While type 2 diabetes accounts for more than 90% of all cases and is closely linked to lifestyle and socioeconomic factors, type 1 diabetes affects an estimated 9.5 million people globally, a figure that has grown by around 13% since 2021, according to the most recent IDF data. Both conditions place enormous demands on individuals, families, and healthcare systems.
The Healthcare and Economic Impact of Diabetes
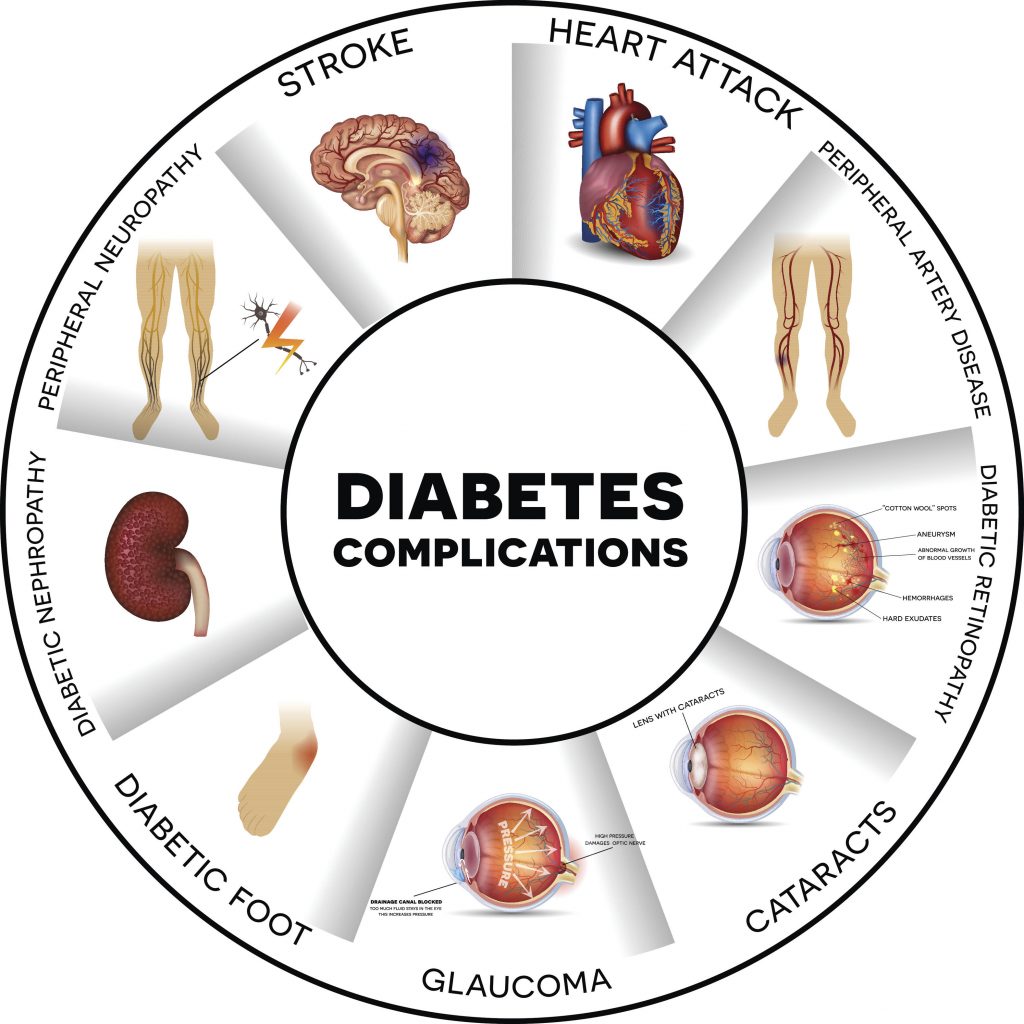
For the people living with it, diabetes is a daily reality that extends well beyond blood sugar management. The condition is associated with a wide range of serious long-term complications. Cardiovascular disease is among the most significant; people with type 2 diabetes face a substantially elevated risk of heart failure compared to those without the condition. Diabetes is also a leading cause of kidney failure, vision loss due to diabetic retinopathy, and peripheral neuropathy, which can lead to pain, reduced mobility, and in severe cases, limb amputation. These complications profoundly affect quality of life and, in many cases, life expectancy.
The economic impact of diabetes is equally significant. The IDF estimates that diabetes-related health expenditure has surpassed one trillion US dollars globally, a staggering increase over the past two decades. This figure encompasses direct healthcare costs including medication, monitoring, and management of complications, as well as indirect costs such as lost productivity. For lower-income countries, where a large proportion of undiagnosed diabetes is concentrated, the financial strain on already stretched healthcare systems is particularly acute.
The human and economic costs of diabetes are not static, they are growing. Without significant advances in prevention, early detection, and treatment, the trajectory points toward an increasingly unsustainable burden on individuals and societies alike.
The Limitations of Current Diabetes Treatments
Existing treatments for diabetes have transformed the lives of millions of people and continue to be essential tools for managing the condition. Insulin therapy, in particular, has been a lifesaving advancement for people with type 1 diabetes, enabling them to regulate blood glucose and avoid acute complications. For type 2 diabetes, a range of medications alongside lifestyle interventions can meaningfully slow progression and reduce complication risk.
However, effective management is not the same as a cure. Insulin therapy requires lifelong daily administration, continuous blood glucose monitoring, and careful dose adjustment resulting in a significant and unrelenting demand on patients. Even with optimal management, the risk of long-term complications remains.
Islet transplantation offers the possibility of restoring the body’s own insulin production, and in successful cases can significantly reduce or eliminate insulin dependency. But this approach is constrained by the availability of donor tissue, which cannot be scaled to meet the needs of the global diabetic population. It also typically requires patients to take immunosuppressive drugs indefinitely to prevent rejection, and these medications carry their own serious long-term risks. The gap between what current new diabetes treatments can offer and what patients truly need remains significant.
The Role of Diabetes Research in Developing New Therapies
The limitations of existing treatments have focused considerable scientific and medical attention on finding better solutions. Diabetes research today encompasses a wide range of approaches, from immunotherapy and beta cell regeneration to gene editing and stem cell-based therapies, with the ultimate goal for many researchers being a functional cure, one that restores the body’s own ability to produce and regulate insulin, rather than requiring external management indefinitely.
Type 1 diabetes research has historically driven much of the foundational science in this area, given the completeness of beta cell loss in that condition. But type 2 diabetes research is increasingly focused on the same cellular mechanisms, as evidence accumulates that beta cell dysfunction plays a central role in type 2 as well. Advances in one area frequently have implications for the other, and the most promising research directions (particularly those involving stem cells) are being developed with both conditions in mind.
Funding for diabetes cure research has grown substantially in recent years, with government agencies, academic institutions, and private biotechnology companies all contributing to an expanding body of work. The question for many researchers is no longer whether a functional cure is possible, but how quickly it can be brought safely and affordably to the patients who need it.
Advances in Type 1 Diabetes Research and the Path Toward a Cure
Among the most significant recent advances in type 1 diabetes research are those involving stem cell therapy. New diabetes research suggests it is possible to generate insulin-producing beta cells from induced pluripotent stem cells (iPSCs), which are reprogrammed adult cells that can be directed to become virtually any cell type in the body. This has opened a pathway to beta cell replacement that does not depend on organ donation and can in principle be produced at scale.
Several research programs are now progressing toward or through clinical trials targeting a cure for type 1 diabetes using cell-based approaches. The goal is to restore functional beta cell mass in patients whose own cells have been destroyed by the immune system, enabling the body to regulate blood glucose naturally, without insulin injections. Achieving this without the need for immunosuppressive drugs remains one of the central challenges and a key focus of ongoing diabetes cure research.
How RMS Is Contributing to Diabetes Cure Research
Regenerative Medical Solutions (RMS) is at the forefront of iPSC-based diabetes research, developing a stem cell therapy designed to address the limitations of both existing treatments and other approaches currently in development. RMS is building on over two decades of research from Dr. Jon Odorico’s laboratory at the University of Wisconsin. The biotechnology company has developed a proprietary technology for producing Islet-Like Clusters (ILCs), cell clusters that replicate the insulin-regulating function of healthy human pancreatic islets.
RMS’s approach is designed to be scalable and accessible. It does not require organ donation, does not use embryonic stem cells, and is being developed to work across all blood types, with the potential to serve a broad patient population with both type 1 and type 2 diabetes. Critically, the therapy is being developed without the need for heavy immunosuppressive drugs or an implantable device, addressing challenges that have limited other approaches.
The company’s research is validated by a strong intellectual property portfolio, including multiple issued patents, and has received grant funding from the National Institutes of Health (NIH). RMS is currently in preclinical development, preparing an Investigational New Drug (IND) submission for entrance into human clinical trials; an important milestone on the path toward bringing a prospective diabetes cure to the patients who need it most.
To learn more about RMS’s diabetes research or to explore collaboration and partnership opportunities, contact our team.
Frequently Asked Questions About the Global Impact of Diabetes
How many people have diabetes worldwide? According to the International Diabetes Federation’s 2025 Diabetes Atlas, approximately 589 million adults aged 20–79 are currently living with diabetes globally, that’s around one in nine adults worldwide. Other estimates, including a 2024 Lancet study, put the figure at more than 800 million when a broader age range is included. More than four in ten of those people are estimated to be undiagnosed.
Is the number of people with diabetes growing? Yes, significantly. The IDF projects that the number of adults living with diabetes could reach around 853 million by 2050, an increase of nearly 50% from current levels, driven by factors including aging populations, urbanization, and rising rates of obesity.
What are the most serious complications of diabetes? Diabetes is associated with a range of serious long-term complications including cardiovascular disease, kidney failure, vision loss, and nerve damage.
Why isn’t insulin a cure for diabetes? Insulin therapy is an effective and lifesaving treatment for managing blood glucose, but it does not address the underlying cause of diabetes (the loss or dysfunction of insulin-producing beta cells in the pancreas). Patients must manage their insulin intake continuously and remain at risk of long-term complications.
What is the difference between type 1 and type 2 diabetes research? Type 1 diabetes research has historically focused on the autoimmune destruction of beta cells and how to replace or restore them. Type 2 diabetes research encompasses a broader range of metabolic factors, including insulin resistance and progressive beta cell dysfunction. Increasingly, advances in type 1 research, particularly stem cell-based beta cell replacement, are being explored for their relevance to type 2 as well.
Is a cure for type 1 diabetes possible? A cure for type 1 diabetes has long been the goal of stem cell researchers, and cell-based approaches now represent one of the most promising avenues for achieving it. By generating insulin-producing beta cells from induced pluripotent stem cells, researchers aim to restore the body’s natural ability to regulate blood glucose, potentially eliminating the need for insulin injections. Several programs, including RMS’s prospective therapy, are working to bring this vision to clinical reality.
