The Science Behind Our Stem Cell Therapy for Diabetes
Stem cell therapy for diabetes aims to treat the underlying cause of the disease rather than simply managing its symptoms. Instead of relying on lifelong insulin therapy, this approach focuses on restoring the body’s natural ability to regulate blood sugar by replacing the cells responsible for producing insulin.
Regenerative Medical Solutions is developing a stem cell therapy for diabetes designed to generate new insulin-producing cells from induced pluripotent stem cells (iPSCs). These cells have the potential to replace damaged or destroyed pancreatic beta cells and restore normal insulin production. This work is part of the broader field of regenerative medicine, which focuses on repairing or replacing damaged tissues using advanced biological technologies.
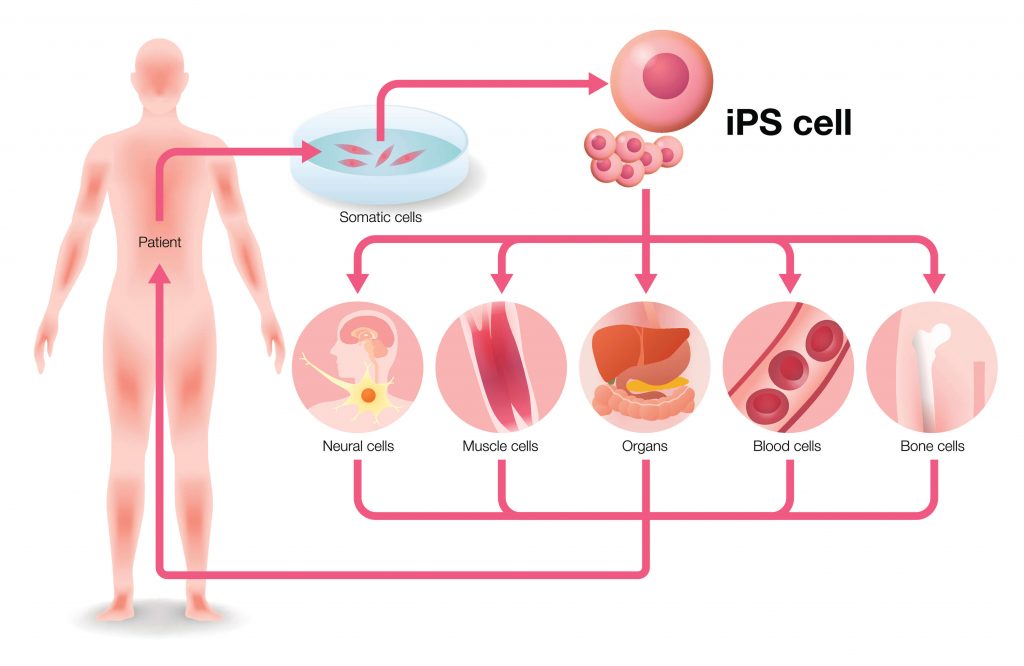
Key Takeaway: How Stem Cell Therapy for Diabetes Works
Stem cell therapy for diabetes aims to restore insulin production by replacing damaged pancreatic beta cells. Using induced pluripotent stem cells (iPSCs), researchers can generate new insulin-producing cells that may help regulate blood glucose levels naturally. This approach, known as beta cell replacement therapy, focuses on restoring the body’s own ability to produce insulin.
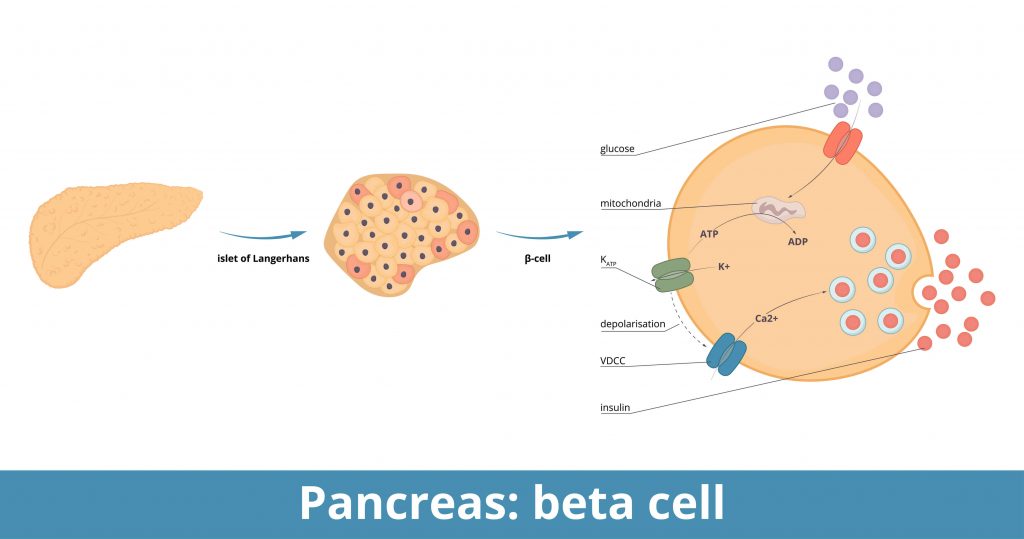
Why Diabetes Occurs: The Loss of Pancreatic Beta Cells
In a healthy pancreas, specialized structures known as pancreatic islet cells regulate blood sugar levels. Within these islets are pancreatic beta cells, which produce insulin, the hormone responsible for allowing glucose to enter cells and be used for energy.
In people with diabetes (particularly type 1 diabetes) the immune system destroys these insulin-producing cells. As the number of functioning beta cells declines, the body can no longer produce enough insulin to regulate blood glucose levels. Without insulin, glucose accumulates in the bloodstream, leading to chronic hyperglycemia and long-term complications.
Current treatments for diabetes typically focus on replacing the missing insulin through injections or pumps. While these therapies are lifesaving, they do not restore the body’s natural insulin regulation. A different approach involves replacing the lost pancreatic beta cells themselves, allowing the body to once again produce insulin in response to blood sugar levels. This concept forms the basis of beta cell replacement therapy.
What Are Induced Pluripotent Stem Cells?
Induced pluripotent stem cells (iPSCs) are adult cells that have been reprogrammed to behave like embryonic stem cells, allowing them to develop into many different types of specialized cells in the body.
Among the most important advances in regenerative medicine has been the discovery of induced pluripotent stem cells (iPSCs).
Induced pluripotent stem cells are created by reprogramming adult cells (such as cells taken from blood or skin) into a pluripotent state. In this state, the cells regain the ability to develop into many different cell types found throughout the body.
Because iPSCs originate from adult tissues rather than embryos, they avoid many of the ethical concerns associated with embryonic stem cells. In addition, they provide researchers with a flexible and scalable source of stem cells that can be expanded in the laboratory and directed to become specific types of specialized cells.
For diabetes research, iPSCs offer a powerful opportunity: they can be guided to become pancreatic beta cells, the insulin-producing cells that are lost in the disease.
How Stem Cell Differentiation Creates Insulin-Producing Cells
Transforming stem cells into functional pancreatic beta cells requires a process known as stem cell differentiation. During this process, scientists carefully guide pluripotent stem cells through a series of developmental stages that mimic the natural formation of pancreatic cells during human development.
By exposing stem cells to specific biological signals and growth factors, researchers can direct them toward becoming pancreatic cells and ultimately insulin-producing cells capable of responding to glucose levels.
This process of stem cell differentiation allows researchers to generate large numbers of beta-like cells in the laboratory. These cells are designed to function similarly to the beta cells found in healthy pancreatic islets, producing insulin when glucose levels rise.
Beta Cell Replacement Therapy for Diabetes
The ultimate goal of generating insulin-producing cells from stem cells is to enable beta cell replacement therapy. In this approach, laboratory-produced pancreatic beta cells are introduced into the body to replace the cells that have been destroyed.
Once established, these new cells may be able to sense changes in blood glucose levels and release insulin accordingly, helping restore natural metabolic control.
Instead of supplying insulin externally, beta cell replacement therapy seeks to restore the body’s own insulin-producing system.
Avoiding the Need for Immunosuppressant Drugs
Traditional approaches to beta cell replacement, such as transplantation of donor pancreatic islet cells, typically require patients to take lifelong immunosuppressant drugs to prevent the immune system from rejecting the transplanted cells. While these medications can help protect transplanted cells, they also suppress the immune system and may increase the risk of infections and other complications.
Our stem cell therapy for diabetes focuses on generating insulin-producing pancreatic beta cells from induced pluripotent stem cells (iPSCs). By developing resilient, functional beta cells through its proprietary stem cell platform, RMS aims to replace damaged cells and restore natural insulin production without requiring patients to rely on lifelong immunosuppressant medications.
Advancing Stem Cell Therapy for Diabetes
Regenerative Medical Solutions is advancing this field through research focused on producing insulin-producing cells from induced pluripotent stem cells and developing approaches that may support long-term restoration of insulin production.
While stem cell therapy for diabetes is still under development, continued progress in regenerative medicine offers the potential to transform how diabetes is treated. By replacing the cells responsible for insulin production, this approach aims to move beyond managing the disease and toward restoring the body’s natural metabolic function.
Frequently Asked Questions
Stem cell therapy for diabetes aims to restore insulin production by replacing damaged pancreatic beta cells with new insulin-producing cells generated from stem cells.
Induced pluripotent stem cells (iPSCs) are adult cells that have been reprogrammed to behave like embryonic stem cells, allowing them to develop into many different cell types.
Beta cell replacement therapy is a regenerative medicine approach that seeks to restore insulin production by replacing damaged pancreatic beta cells with healthy cells capable of producing insulin.
Stem cells are guided through a process called stem cell differentiation, where scientists expose them to specific biological signals that direct them to become pancreatic beta cells capable of producing insulin.
Contact RMS
Contact Regenerative Medical Solutions to learn more about the work of Dr. Odorico, our team of scientists, and our stem cell therapy for diabetes.
